
It is a disease caused by a parasite that infects a very certain type of female mosquito called the Anopheles mosquito. It is spread through the bite of this mosquito and can be a fatal disease if left untreated.
There are four kinds of malaria parasites that infect humans: Plasmodium falciparum, Plasmodium vivax, Plasmodium ovale, and Plasmodium malariae.
Malaria is not a contagious disease, it can not spread from person to person like the flu or a cold. Casual contact with a person affected with malaria is safe and will not infect other person that does not have malaria.
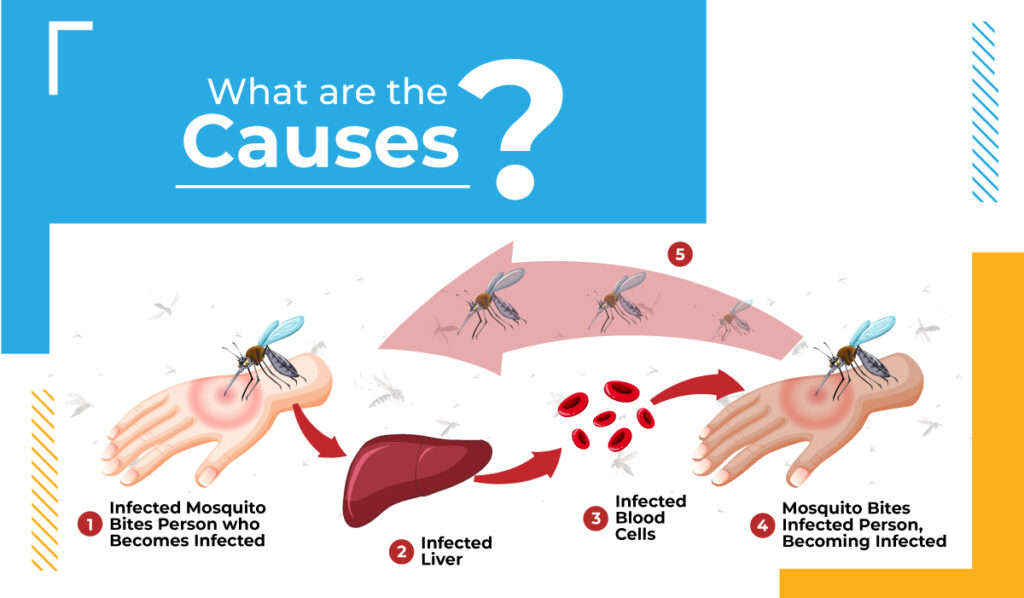
What are the causes?
Typically, an infected individual receives a bite by the infectious female Anopheles mosquito, and the insect takes in a little quantity of the contaminated blood.
Once the anopheles mosquito has been infected with the parasite, the parasite multiplies and mixes with the mosquito’s saliva. When the mosquito bites into its victim, it injects that saliva into the human body causing malaria. Upon infection, the parasites grow in the liver before spreading to the red blood cells and infecting the host.
It can be transmitted very rarely through blood transfusion, organ transplant, or the shared use of needles and syringes. A pregnant mother with malaria can transfer it to her unborn child or during delivery called congenital malaria.
What are the symptoms?
The symptoms can begin as early as seven days after being bitten and up to four weeks afterward. Very rarely, symptoms may appear up to a year later depending on the type of parasite. Most commonly they are,
- Fever
- Chills
- Sweats
- Headaches
- Diarrhea, nausea and vomiting
- Body aches
- General malaise
- Elevated temperatures
- Perspiration
- Anemia
- Weakness
- Enlarged spleen
- Mild jaundice
- Enlargement of the liver
- Increased respiratory rate

Complications
Severe malaria can cause serious organ failure and other abnormalities in the patient’s blood or metabolism. Severe malaria can also cause the following:
- Cerebral malaria which can lead to seizures, abnormal behavior, lack of consciousness, and coma
- Due to hemolysis (destruction of red blood cells), severe anemia can occur
- Hemolysis can cause hemoglobinuria which is hemoglobin in urine
- Inflammation in the lungs inhibits oxygen exchange. It is called Acute respiratory distress syndrome (ARDS)
- Abnormalities in blood coagulation
- Low blood pressure caused by cardiovascular collapse
- Acute kidney injury
- Infection of more than 5% of the red blood cells by the malaria parasite called Hyperparasitemia
- Metabolic acidosis (excessive acidity in the blood and tissue fluids), often in association with hypoglycemia
Treatment for severe malaria has to start right away and be vigorous.

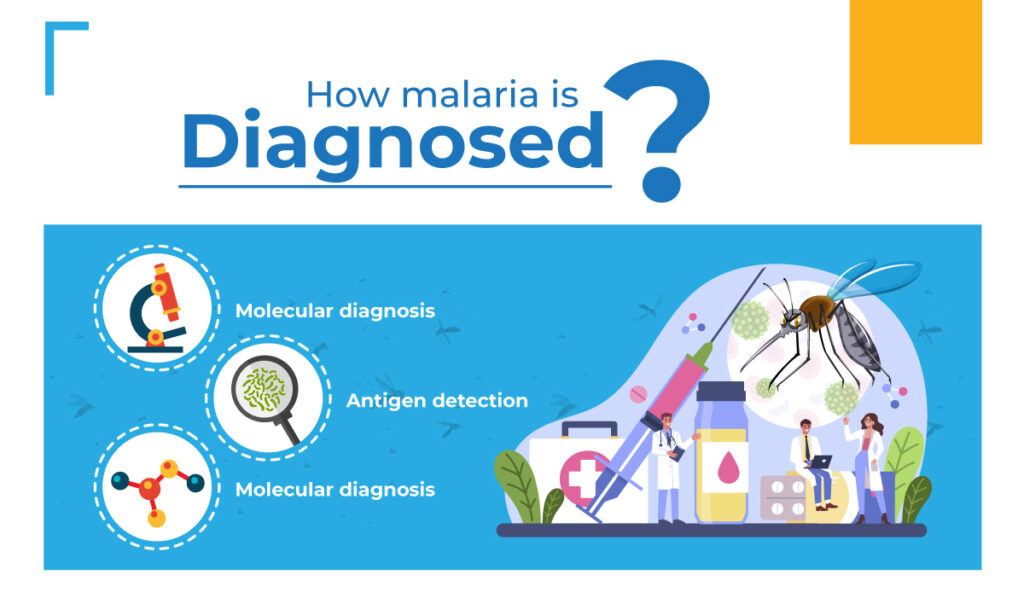
How is malaria diagnosed?
Symptoms of malaria, such as fever, sweats, and chills, are quite general and can be mistaken for other conditions. To confirm whether it is malaria or not, a lab test is necessary.
Microscopic diagnosis: A drop of the patient’s blood is spread out as a “blood smear” on a microscope slide and it is examined under a microscope. Before the specimen is observed, it is stained to give the parasites a distinct appearance.
Antigen detection: Antigens are detected with various kits for malaria parasites. The results are provided in 2-15 minutes. These “Rapid Diagnostic Tests” (RDTs) are a useful alternative to when microscopic diagnosis is not available. It is recommended to follow up RDTs with microscopy to confirm the results, the species and to know the amount of red blood cells infected. RDTs save time by determining if the patient has malaria or not.
Molecular diagnosis: Parasites are detected using polymerase chain reaction (PCR). It is useful for confirming the species of the malarial parasite but it is too slow of a process to establish diagnosis of malaria infection.
What is the treatment?
If you are afraid that you have malaria, you can get your blood tested to see if there are any parasites in it. Malaria is a disease that can be cured if treated early and properly through available antimalarial drugs. The drugs used to prevent malaria have been shown to be safe and well-tolerated for long term use. The type of prophylactic medicine will depend on the type of malaria parasites in the area and drug resistance. A doctor should be consulted or health staff to determine the type of medicine to be used for prophylaxis.
Some medications used for prophylaxis are atovaquone-proguanil, chloroquine and hydroxychloroquine, doxycycline, mefloquine, primaquine and tafenoquine.
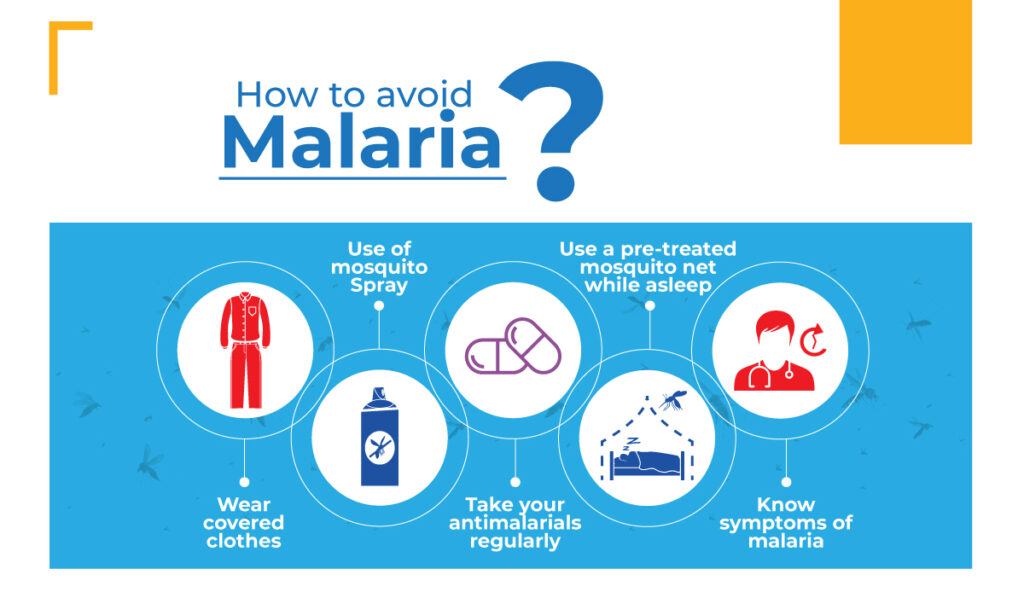
How to avoid malaria
Malaria can be prevented by
- Keeping mosquitoes from biting you by wearing insect-repellent and fully covered clothing.
- Eliminating places around your home where mosquitoes breed, like small ponds or areas where there is waterlogging.
- Spraying insecticides on your walls to kill mosquitoes.
- Sleeping under bed nets, particularly those treated with insecticide.
- Taking medication prior to traveling to areas where malaria is prevalent.
- Vitamin A is known to boost immunity, improve the ability to fight off infection and may help the body to clear out the malaria parasite more quickly.

There are no vaccines currently to prevent malaria approved for human use. Though scientists are working on it, the malaria parasite has a complicated life cycle, constantly changing its surface and antigens which makes developing a vaccine very difficult. The search for a malaria vaccine is one of the most important research projects in public health.
REFERENCES:
Children Who Get Vitamin A May Be Less Likely to Develop Malaria. (2021, July 7). Johns Hopkins Bloomberg School of Public Health.
https://publichealth.jhu.edu/2015/children-who-get-vitamin-a-may-be-less-likely-to-develop-malaria
CDC – Malaria – Diagnosis & Treatment (United States) – Diagnosis (U.S.). (n.d.). https://www.cdc.gov/malaria/diagnosis_treatment/diagnosis.html#:~:text=Malaria%20parasites%20can%20be%20identified,the%20parasites%20a%20distinctive%20appearance.
Malaria – Chapter 4 – 2020 Yellow Book | Travelers’ Health | CDC. (n.d.). CDC.gov. https://wwwnc.cdc.gov/travel/yellowbook/2020/travel-related-infectious-diseases/malaria#:~:text=The%20most%20common%20adverse%20effects,nausea%2C%20vomiting%2C%20and%20headache.
Albright, T., Binns, H. J., & Katz, B. Z. (2006, March 8). Side Effects of and Compliance with Malaria Prophylaxis in Children. Journal of Travel Medicine; Oxford University Press. https://doi.org/10.2310/7060.2002.30091






